 CSF leaks can also be linked to meningoencephalocele – this is a uncommon condition that is present at birth. Leaks are usually due to a fracture in the skull, feebleness of the brain covering (dura), intracranial surgery or development of a brain tumor. Although a cerebrospinal fluid leak is uncommon, the CSF can leak through the brain covering and into the nose area. 
The brain continuously produces CSF and reabsorbs it back into the blood system. CSF is an essential fluid that keeps the cerebral tissue from injury and infections. This liquid flows through the ventricles in the brain. One should consider alternative methods to nasal screening in patients with known prior skull base defects, history of sinus or skull base surgery, or predisposing conditions to skull base erosion.Cerebrospinal Fluid Leaks Cerebrospinal Fluid Leaks – AboutĬSF, otherwise known as Cerebrospinal Fluid is a see-through, colorless liquid that pads the brain. This case of iatrogenic CSF leak from nasal swab testing for COVID-19 illustrates that prior surgical intervention, or pathology that distorts normal nasal anatomy, may increase the risk of adverse events associated with nasal testing for respiratory pathogens, including COVID-19. Such complications have not been well described in the existing literature. 2 However, adverse events may still occur owing to complex and delicate anatomy. High-quality instruction on how to properly obtain an adequate nasopharyngeal specimen for testing is available. As the number of daily COVID-19 nasal and nasopharyngeal swab specimen collection procedures increases, a greater burden is placed on the health care system to properly train clinicians and even the general public to safely perform nasal and nasopharyngeal swab testing. 5 Although it is now routine in the US to rule out COVID-19 prior to elective surgeries, for many hospital admissions, and for symptomatic individuals, additional testing may help contain the spread of COVID-19. We therefore theorize that the swab itself did not result in a violation of the bony skull base, but rather the invasive test caused trauma to the patient’s preexisting encephalocele.Ĭapacity for COVID-19 testing is increasing in the US, with plans to ramp up to as many as 6 million tests per day by the end of 2020. 3 Idiopathic intracranial hypertension is a risk factor for meningocele formation, 4 and this patient had an undiagnosed skull base defect at the fovea ethmoidalis that was present on imaging dating back to 2017. Of prior reported iatrogenic CSF leaks from intranasal procedures, surgical trauma at the cribriform plate is the culprit in CSF leaks 8% to 58% of the time. To our knowledge, this is the first report of an iatrogenic CSF leak after a nasal swab for COVID-19. The patient was admitted postoperatively for neurological monitoring and lumbar drain management. After reduction of the encephalocele, a skull base defect in the fovea ethmoidalis was repaired with a combination of acellular human dermal matrix and a poly(D,L-lactic) acid. An encephalocele was identified in the right anterior ethmoid cavity ( Figure 2). At the beginning of the procedure, intrathecal fluorescein was infused through a lumbar drain. The patient was admitted to the hospital for endoscopic surgical repair. The 2017 CT diagnosis was paranasal sinus disease but not an encephalocele. Comparing these images to findings on CT performed in 2017 revealed that the encephalocele dated at least to that time ( Figure 1). Computed tomography (CT) and magnetic resonance imaging (MRI) identified a 1.8-cm encephalocele extending through the right ethmoid fovea into the middle meatus and a right sphenoid wing pseudomeningocele. 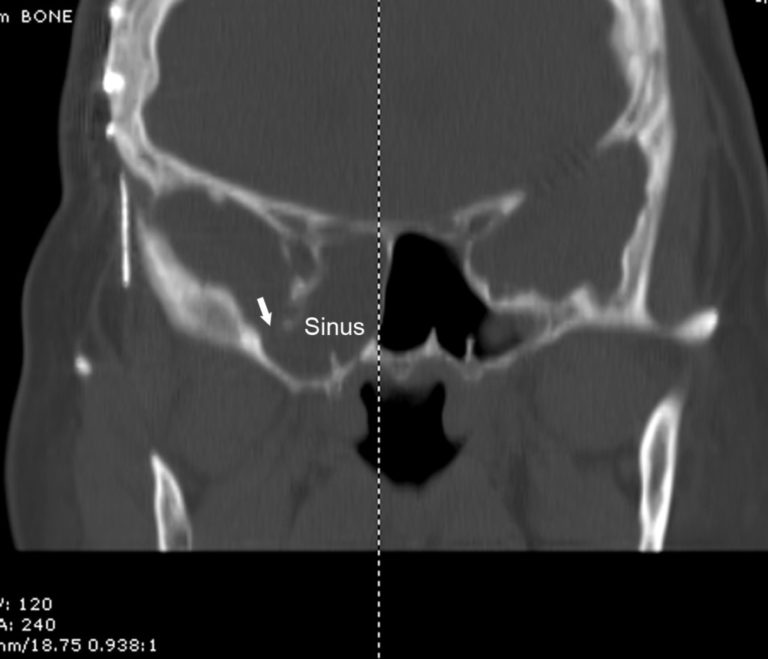 
The nasal drainage tested positive for β 2-transferrin. Flexible nasopharyngoscopy revealed a mass in the right anterior middle meatus, but did not identify the source of the fluid. Physical examination revealed clear rhinorrhea from the right side. The patient’s medical history was notable for idiopathic intracranial hypertension and removal of nasal polyps over 20 years before presentation. Shortly after, she developed unilateral rhinorrhea, headache, and vomiting. The patient had recently completed nasal COVID-19 testing for an elective hernia repair. Shared Decision Making and CommunicationĪ woman in her 40s presented with unilateral rhinorrhea, metallic taste, headache, neck stiffness, and photophobia.Scientific Discovery and the Future of Medicine.Health Care Economics, Insurance, Payment.Clinical Implications of Basic Neuroscience.Challenges in Clinical Electrocardiography. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
